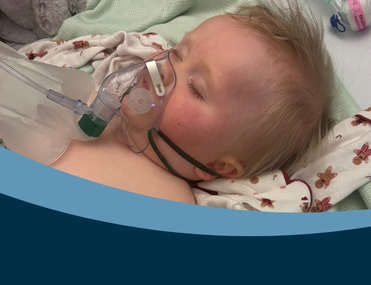
She was pale and her skin was very mottled, but at first doctors believed Holly-May just had a viral infection.
In fact she had contracted meningococcal type b meningitis and septicaemia. Thankfully the brave tot pulled through. Mother Meghann takes up their story.
“Holly-May was 15-weeks-old when she became unwell on the 5th of April 2013. Holly had previously been in hospital and was treated for an unknown infection so we knew the general signs to look out for. She had a very high temperature pushing 40 and was not always relieved by paracetamol. She was pale and her skin was very mottled. She was unsettled and was crying a lot. She was refusing to drink her milk and we were struggling to keep her hydrated. She had diarrhoea but at this stage was not vomiting.
As her parents we knew something wasn't right and took her straight to the doctors. They were fantastic. The doctor could see a mile off that Holly was unwell and sent her by non-emergency ambulance to hospital. After about an hour Holly was assessed by a doctor and we were told that, as she wasn't vomiting, they believed it was just a viral infection that she would fight off herself.
Due to her previous history of infection we knew this wasn't the case and asked for a second opinion. We asked for blood tests to be done to check for infection but we were told we were just being over cautious and were sent home the same evening.
Over the next two days Holly remained unwell and our worries grew. We kept monitoring her and treating her with paracetamol and brufen. By Monday the 8th we became very concerned. Overnight Holly had deteriorated and she was now vomiting and completely refusing any liquids. She was very drowsy and hard to wake and incredibly irritable. She would whimper and let out a high pitched shriek when touched and was no longer supporting her own head."
Straight over to the doctor’s surgery
“We took her to the doctors but while waiting to be seen we went across the road to the pharmacy to see if we could get anything to help with her dehydration. We now know that if it wasn't for the fast action of the people involved next our precious girl wouldn't be with us today. The pharmacist examined Holly and was very concerned. He walked us straight over to the doctors’ surgery and asked for us to be seen straight away.
The same doctor who saw her three days earlier took us straight into his room and examined her. He said she was severely dehydrated as her CAP refill should have been 1-2 and was 3+ and rang through to the children's ward she had been discharged from and referred her back. He told us that he couldn't believe she had been discharged at all.
We were taken to an empty room to wait for the transport ambulance when I noticed Holly wasn't breathing properly - she was struggling to take breaths. Holly's dad went and got a doctor and they rang for a rapid response ambulance. We were told she was okay but they were giving her some oxygen to be safe. When the ambulance arrived we were blue lighted to the hospital where we were taken to a side room right away.
From there everything is slightly blurred and it went so fast. She was kept on oxygen and examined by a lot of doctors and nurses. The main issue was her dehydration. Holly was in a bad way. She was cannulated and given injections of fluid while also having a drip of fluid going through. Her temperature kept rising and nothing was bringing it down."
Medical professionals crowded round her bedside
“Two anaesthetists came to see her and us. At one stage there were over 10 medical professionals crowded round her bedside. They started her on antibiotics and we asked what was causing Holly to be so unwell, but they told us at this stage she was too unwell for tests and were concentrating on keeping Holly stable. The anaesthetists told us that they had done all they could to improve her and that if they gave her any more fluid it would become too difficult for her heart to pump it all round her body. They said if her SATs didn't start to improve we would need to agree to let them take Holly to theatre and put her under so they could ventilate her and allow her body to rest while the machines did the work for her so they could give her more fluid.
They also wanted to put an arterial line in as well as the cannula, as the fluid and medicine were the only things keeping her alive and they were worried in case it failed. The doctors and nurses tried their best to keep us calm and we were told that taking her to theatre now was the safest option as they had time and wouldn't be rushing."
Said goodbye and kissed her
“We said goodbye and kissed her in a state of complete shock and disbelief. She was very quickly ushered away. We later found out her heart had started to fail and she had to be resuscitated. We just couldn't believe that 72 hours after being sent home she was back and now on life support.
When the procedure was finished we were allowed in to see her. Her eyes were taped shut, she was wrapped in tin foil and looked so frail. They had given her morphine and were keeping her fully sedated while the machine did all the work so she could build her strength up. She'd been given more fluid now and it was just a waiting game. Seeing her like that is a moment I will never be able to forget.
It was a nightmare but I was already awake. It was so surreal, almost like I was watching from above. Not my little girl, it couldn't be.
Our local hospital didn't have the facilities she needed, so she was transferred to the Royal Manchester Children's Hospital. We weren't allowed in the ambulance with her as there was too much equipment. We were told it would take two hours to load everything up in the ambulance and another two hours to unload everything on the other side as well as the journey itself, so we were told to go home and get some rest.
Seeing our daughter like that and then walking away and leaving her was very hard. I genuinely didn't know if I was going to see her alive again and I wouldn't wish that heartbreak on anyone. When we got up to the hospital it took a while for us to see her but when we did she looked very unwell. She had low levels of potassium, which was what was causing the problems with her heart.
Over the next two days while in intensive care Holly-May was still too poorly to have any invasive tests done to check what was causing her to be so ill. She had some bloods done which showed incredibly high levels of infection. She was on a fluid drip and two antibiotics, as well as potassium to help her heart.
Holly's Nana was sitting with her when Holly’s leg started to go blue and her pulse slowed. Doctors tried all sorts, including removing the arterial line from her groin, but nothing made any improvement. We were warned she could lose her leg. In desperation Holly's Nana picked her up and, thank heavens, the blood flow started to return."
So many questions
“Holly-May was taken off the ventilator after breathing more and more on her own and was transported back to our local hospital. They became increasing concerned due to the severe pain she was in with her head and neck and the fact that along with the inability to support her head the back of her skull would stiffen against her back when she was picked up. They decided she needed a lumbar puncture, which confirmed she had meningitis - meningococcal type B septicaemia. But they sent her home? But she didn't have a big purple rash? I had so many questions but there wasn't time to sit and wonder, we had to get her better.
All Holly's close family members were given antibiotics and Holly continued treatment, although unfortunately she wasn't improving. Her temperatures and infection levels were still rising and weren't responding to treatment. She had become so anaemic that she needed a blood transfusion but unfortunately along with how desperately her body needed the transfusion her body also rejected it and had to have it repeated. Luckily the second time was a success.
Holly's case was sent to the microbiologists who then decided on a concoction of different antibiotics to fight off the meningitis. But still, after over nine days on antibiotics, Holly's infection levels and symptoms were still rising. She had swelling around her eyes and her skull. She was sent for a CT Scan that revealed Holly had swelling on her brain. We didn't know what the future was going to be for her and whether she would have brain damage, hearing loss or any other number of complications.
We are so lucky that almost two years on we have a very happy, healthy, cheeky little girl who has defied all the odds. We are very thankful but also very certain of one thing - there has to be a vaccine! Not all children are as lucky as Holly-May and no one else's children need to suffer. Together we can make a difference and help stamp out meningococcal type B. Through all of Holly's struggle and fight to win her battle the vaccine was approved and waiting to be used.”