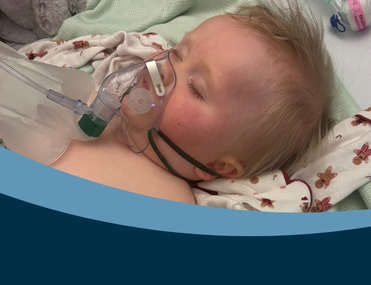
One Friday afternoon just before her second birthday, Jasmine began feeling unwell.
She told her mum that her head and neck were hurting; she became weak and lay on the sofa not wanting to move.
Later that day, Helen noticed a rash developing on Jasmine’s body, and it was spreading rapidly.
“Warning bells were ringing,” said Helen, “but meningitis is a bit like a lightning strike; you never think it will happen to you.”
Helen gave Jasmine some medicine, but her temperature kept rising. On Saturday morning, Helen called the out-of-hours doctor and made an appointment for the Sunday morning. On Saturday evening Jasmine’s temperature continued to rise and soared over 100 degrees.
Helen was so worried that she dialled 999, and a paramedic arrived shortly after.
“He took Jasmine’s temperature and checked her over. He took a glass and rolled it over her rash, but they disappeared so he said it ‘couldn’t be meningitis’ and discouraged us from going to A&E. I wish I hadn’t listened.”
Extremely ill
The following morning, Jasmine began to deteriorate rapidly. By the time she arrived at the hospital for the out of hours doctor appointment, she was clearly in a very serious condition.
“Her skin had gone ‘waxy’; it really looked just like church candlewax”, said Helen, “Her arms and legs were blotchy where her circulation was shutting down, and her eyes were rolling in her head. I was so scared.”
A doctor tended to Jasmine straight away and rushed her straight into A&E.
“The doctor was great; she didn’t mention any suspicions of meningitis so we didn’t panic. She was all but running though, so I knew things weren’t okay.”
Jasmine was taken straight to the resuscitation room, where four doctors and six nurses immediately started working on her. She did not have a lumbar puncture as, by now, it was very obvious to the medical staff that Jasmine had contracted meningitis.
“The doctors struggled to get IV lines into her veins and only managed one, they couldn’t find another. I lay over her, telling her to look at me and not to fall asleep. I kept telling her to stay with mummy and that the doctors were going to stop it hurting soon.”
Lucky to be alive
The doctors were forced to squeeze the IV bags in order to get the medicine into Jasmine as quickly as they could. Then, it was just a case of waiting to see if it would work. Fortunately it did.
“By late afternoon, Jasmine was talking to me again. She started pointing out the cute animals on the walls; she was being quite coherent.”
Jasmine remained in resuscitation in case she took a turn for the worse. When she showed no signs of deterioration, she was transferred to a ward and put in an isolation room. After a few days, she was finally well enough to go home; returning to the hospital for the remainder of her treatment.
Helen does not underestimate how close she was to losing her daughter.
“We were so very lucky. It brings tears to my eyes when I think about how I nearly lost my little girl; the doctor said that if we’d have been just fifteen minutes later, she would probably have died.
My heart goes out to all the families who have lost their loved ones. I know two people who have died from meningitis, and I know just how lucky we are that Jasmine recovered completely with no lasting damage.”
Don’t wait for a rash
Contrary to popular belief, a rash does not appear in all cases of meningococcal disease, and if it does it usually appears late; by which time, victims are often already seriously ill.
“In Jasmine’s case, she did have a rash but her diagnosis was still almost missed. She was covered in a rash all over her body, but only three of the spots were the pin-prick spots indicating the septicaemic rash,” said Helen.
She still regrets not trusting her parental instincts at the time Jasmine became ill; wishing that she had insisted that the paramedic took Jasmine to hospital.
“I know now that A&E’s prioritise children and my advice to everyone is to trust your instincts and make the medical staff listen to you.
The doctors are the experts in medicine; but we are the experts when it comes to our loved ones. We are the ones who know them and know how they usually react to illness.
"I would never have been able to forgive myself for waiting for the out-of-hours appointment if I’d lost my daughter. It’s not just parents who need to be aware either; paramedics need more education on the signs and symptoms so that they act quickly.”